Overweight - how much does it cost and what to do about it?
The dynamics of overweight and obesity in the world
The problem of overweight and obesity in recent decades has been highlighted in the health systems not only of the most developed countries of the world, but also of middle and low income countries. Thus, according to WHO estimates, the proportion of overweight adults (body mass index, BMI4> 25) in developed countries averages from 35 to 55%, and in some countries (USA, Canada, Australia, Great Britain, New Zealand, Greece ) already reaches 65-70%. Obesity (BMI> 30), although less common, also covers a significant part of the population - an average of 15-20%, in the US - about 40%.

According to the WHO, in 2005 about 1.6 billion of the adult population of the planet suffered from overweight, of which at least 400 million people were from obesity. According to forecasts, by 2015 these figures will increase to 2.3 billion and 700 million, respectively. Experts are concerned, above all, by the extremely rapid spread of these phenomena throughout the world, observed from about the mid-1970s. For example, only in Great Britain the number of obese people has increased 5 times over the past 25 years. In the United States, a country where overweight is significantly more than half the population, scientists predict a continuation of this trend - by 2020, 77.6% of men will have a BMI higher than 25, and 40.2% will be higher than 30, for women the corresponding figures will be 71,1% and 43.3%, respectively, with the prevalence of the most severe forms of obesity increasing at an especially fast rate.
Obesity is already named in the WHO and OECD documents as a global epidemic or pandemic. In November 2006, WHO convened a special European ministerial conference on obesity, which adopted a number of documents calling on governments of all countries in the region to work together to combat this phenomenon.
Causes of overweight
Historically, indicators of weight and height of a person were used in medicine for a long time, however, they were of interest to health policy primarily as indicators of malnutrition, poor nutrition quality of the population, which as a result became the cause of disease. Only in 1995, WHO established uniform criteria for determining overweight and obesity, recognizing, therefore, the existence of a fundamentally opposite problem. It is interesting to note that if overweight was initially logical to be considered a problem of rich and "well-fed" countries, it later turned out that in countries with moderate and even low income levels, obesity is becoming more and more widespread, often safely adjacent to poverty and malnutrition.
What are the causes of excess weight, and why this phenomenon is spreading at an increasing rate? Of course, the weight of a person, as well as other anthropometric characteristics, varies in any single set, it was and will be at all times. Overweight, such as, for example, tall or short stature, can be inherited from parents to children. However, only genetic factors can not explain the growing obesity in most countries of the world - because then it would be necessary to assume that full people have more children than people with medium and low weight, and in practice there is exactly the opposite trend.
The most common explanation given by physiologists to obesity is the discrepancy in the amount of energy consumed and consumed by man (95-97% of cases of obesity are explained precisely by this reason). At the same time, some researchers focus on the growing caloric content of food, others - on reducing the physical activity of a modern person. The energy imbalance in general is explained by changes in technology: on the one hand, cooking is becoming more and more simple and fast, food itself is relatively cheap, on the other hand, people's lifestyle changes, physical labor is automated, it is replaced by "office" work . The rapid growth in employment in the services sector, urbanization, “motorization” - all these factors, of course, contribute to the growth of BMI. In developed Western countries, such factors as growing employment of family women are noted separately. Studies show that in families where the mother works, children are more susceptible to obesity - obviously, this is also the result of irregular nutrition, eating ready-made food, especially fast food (high-calorie food and cheap at the same time).
Selected country studies show a close relationship between BMI and a person's age - in this sense, the growing overweight of the population can be partially statistically explained by the “aging” of many modern economies. However, even more “younger” countries with shorter life expectancy show an increase in BMI, so that such an explanation can hardly be considered exhaustive.
American scientists also note the inverse dependence of overweight and socioeconomic status - people with high incomes are more often more physically active, eat well, smoke less and consume alcohol, etc.
If once a family’s high income meant rich and nourishing food, today everything is the opposite - the poor people eat relatively cheap foods rich in “bad” fats and carbohydrates, the better off can afford an expensive “healthy” diet. It is proved, moreover, that food addictions are inherited by children from their parents, so that obesity is reproduced in the family. The closest interconnection between foreign researchers was able to establish between obesity and the level of education - this factor has the maximum explanatory power in the differences in BMI between individual socio-economic groups, and among educated people there are much less full.
These reasons allowed economists to formulate two main theories in an attempt to explain the obesity phenomenon. The first one is neoclassical, in which the achievement of a certain "ideal" weight is considered as a normal good. With low income and low weight (malnutrition), a rational individual seeks to increase his weight as soon as income starts to grow. On the contrary, starting from a certain threshold level of weight and income, the opposite desire arises - to maintain or reduce weight. Thus, the dependence of weight and income is nonmonotonic. It is important to note that the concept of “ideal weight” itself, although it is actively imposed on society from the outside, is in practice perceived by most people simply as a mean value; people in general tend to compare themselves with others, and not with movie stars. Therefore, the growing weight of the entire population in general shifts the “ideal”, and leads to a further increase in BMI. Similarly, the relative decline in food prices, from the standpoint of the neoclassical approach, ceteris paribus, increases its consumption, which means it contributes to obesity.
Another theory is behavioral, based on the classic work of G. Becker and K. Murphy on rational addiction. Proponents of this theory are trying to apply it to the phenomenon of obesity, explaining the style of nutrition of the individual his preferences. So, they note growing loads at work, which lead to more rare and irregular meals, the habit of eating in a cafe or restaurant, having a snack while running - all this inevitably leads to weight gain.
The consequences of overweight and their evaluation
The effects of overweight and obesity, which economists have traditionally described in terms of costs, are many and varied. Direct and indirect costs are distinguished, and although not all of them can be directly estimated in monetary terms, it is obvious that with an increase in weight above a certain level, an individual’s utility decreases.
Under direct costs understand the losses associated with the treatment of diseases caused by becoming overweight. A special place in the estimates of direct costs occupy epidemiological studies. Opinions of experts are divided when the question arises whether obesity is a disease in itself, however, it has long been known that overweight can cause certain diseases. It is unequivocally proven that overweight increases the risk of coronary heart disease, hypertension, stroke, type II diabetes, osteoarthritis, and certain types of tumors. At the same time, cardiovascular diseases and diabetes steadily occupy the first lines in the ratings of the most “deadly” diseases in high- and middle-income countries, and, according to experts, will retain these positions in 2030. WHO specialists believe that in the next 10 years alone, the number of deaths caused by diabetes will increase by 50% in the world. Thus, it is obvious that obesity, with its increasing prevalence, makes a considerable contribution to the indicators of both morbidity and mortality.
For example, the authors of one of the recently published studies estimate the proportion of growing BMI in the global burden of type II diabetes, 58%, the contribution of obesity to the burden of ischemia is estimated at 21%, for hypertension the same indicator is 39%, from 8 to 32% for various forms of neoplasms, 13% for osteoarthritis. Overall, WHO estimates that overweight is the fifth most important risk factor contributing to the burden of disease in developed countries.
Mortality, as studies show, is also associated with a person's weight, and the dependence of mortality and BMI (within the same age and gender groups) is U-shaped: the lack of weight, as well as its excess, increases the risk of death, other things being equal circumstances A person suffering from obesity at the age of 20 will live on average 5 years less than his peer with a normal weight. The increase in mortality caused by obesity, according to experts, can reverse the general trend of increasing life expectancy, which is observed throughout the world over the past 200 years.
The growing incidence among overweight people naturally leads to an increase in treatment costs. Thus, according to the research corporation RAND, people suffering from obesity spend on services of medical institutions an average of 36%, and on medicines - 77% more than people with normal weight (for comparison, for smokers these figures are 21% and 28%). Thus, it turned out that obesity is much more expensive than traditional bad habits. The direct costs of obesity-related medical care vary from country to country and constitute, according to various estimates, from 5 to 10% of total health expenditure.
The indirect costs of overweight are estimated primarily through the reaction of the labor market. It is important to note the serious problems experienced by overweight people in finding employment - the probability of finding a good job for them is less. This applies particularly to employment in the services sector, which today dominates in all developed economies, because here the employee is more often in direct contact with the client, which means that the appearance of the candidate is important for the employer in hiring. In addition, numerous estimates show that the earnings of full-time workers, ceteris paribus, turn out to be lower than that of their colleagues with normal weight, and to a greater degree these differences are manifested among women. All these facts can speak both about the relatively low productivity of overweight workers, and about possible discrimination on this basis. Thus, from the point of view of the labor market as a whole, the loss of overweight workers can be estimated in terms of wage losses. In addition, they are often absent from work due to illness, more often they draw up an early pension or disability — these costs can also be estimated. In fact, the labor market “punishes” full-time employees.

Some authors emphasize that the consequences for the labor market need to be considered not so much in terms of reducing the productivity of today's workers, but rather in terms of the quality of labor resources in the future. After all, the estimates made for the labor market today include only those already working. Meanwhile, the process of obesity affects children more and more, and research shows that overweight children are less willing and less willing to learn. According to WHO, today every tenth schoolchild in the world is overweight, with childhood obesity affecting not only the United States, but also countries such as South Africa, Italy and other states of Southern Europe. Thus, the problem of the quality of the workforce arises in the long term, and indirect costs are no longer just estimated as today's losses, but as potential losses in the future.
Among indirect costs, there are also psychological ones: the so-called stigmatization, frequent depressive states of obese people. The limitations of their mobility and leisure activities are difficult to estimate in monetary terms, however, there is a decline in the quality of life. Some studies have noted, in addition to dissatisfaction with their appearance, and direct economic losses, especially for women who find it harder to get married. It is proved that with increasing weight decreases the probability of having children.
The indirect costs also include the loss of society from externalities. In terms of economic theory, we can speak about the external effects of obesity - after all, an increase in the incidence rate, a decrease in the productivity and quality of the work force are becoming a problem for the whole society, and not just for an individual. The states in those countries of the world where the problem of overweight is already fully realized are spending more and more money on scientific research in this area, the creation of new drugs and methods of treatment; insurance companies pay for their patients special operations, and it is clear that the burden of expenses ultimately falls on the entire population. At the same time, global economic studies clearly show that the level of public health is a reliable prognostic factor for economic growth, which means that any factors that impair health, become an obstacle to further development. E. Finkelstein and L. Zuckerman, the authors of the new book "The Fattening of America", examining the effects of obesity from macroeconomic positions, talk about reducing the competitiveness of national business, bringing jobs to other countries, weakening the country's defense, increasing taxes for the population and soon going bankrupt national health insurance programs.
Thus, we can talk about the serious negative consequences of obesity - both for the individual and for society as a whole. Hence the need for government intervention, on the basis of both economic and social inefficiency.
Public policy measures
Today, the developed countries of the world spend significant funds on the treatment of obesity and diseases associated with it. Both drug and surgical treatment methods are costly and not always effective, especially in the long term. Therefore, it is primarily about preventive measures - how to prevent the emergence and further spread of obesity?
Since overweight, like smoking, turns out to be one of the most important risk factors for diseases, it is logical to draw here a certain analogy. However, this analogy is rather limited, as in the case of obesity, many of the measures used in the fight against smoking are not applicable. Food, unlike tobacco, is vital for a person, and in itself is neither a bad habit, nor a risk factor for disease. If, in the fight against smoking, the ultimate goal is to ensure that people simply do not start smoking, then there is no such goal.
Differentiated indirect taxes on selected foods are offered as a standard economic measure. As a result, the price structure should change, taxes on “harmful” products are compensated by subsidies to producers / sellers of healthy food. At the same time, experts warn about the danger of such a measure - after all, it is a matter of basic necessities, which means that the tax is likely to be regressive. In the structure of consumption of poor families, a large share is made up of precisely those products that will become more expensive, and vice versa. From the theoretical point of view, the best option would be to introduce a non-linear tax scale, so that at a higher rate the consumption of “excess” food would be taxed, but in practice such a proposal is difficult to implement. Instead, they offer either a differentiated tax depending on the content of individual ingredients (sugar, fat), or by product category, or on all food products. The best approach, according to some experts, is to impose increased VAT on those food producers whose share of value added is higher, that is, the products undergo a longer processing time. However, there are doubts that such complex taxation schemes will prove economically viable.
Direct legislative methods of regulation are proposed in terms of limiting the number of fast food enterprises, their availability (geographic location). Commitments are also being introduced for food producers to post information on calorie, fat, sugar, etc. on the labels. Some experts propose a direct ban or restriction of fast food advertising; banning the sale of fast food, chocolate, carbonated drinks, etc. in schools.
The most promising direction is education (propaganda), especially among children and young people. Among the specific measures: the dissemination of information about the dangers of overweight and obesity, learning the basic principles of proper nutrition. It is primarily about the formation of a culture of nutrition and a generally healthy lifestyle. By analogy with smoking, the task is to achieve changes in society’s attitude towards overweight, to realize that completeness is not just a cosmetic defect, but the cause of many diseases and a possible obstacle to career success and in general in life.
The scale and characteristics of the prevalence of overweight in Russia
Estimates of the prevalence of such phenomena as overweight and obesity, made for Russia, differ depending on the sources. Thus, the WHO data show a level slightly lower than the estimates of specialists from the Institute of Nutrition of the Russian Academy of Medical Sciences (obesity - 24% of the population, overweight - more than 50%. At the same time, both sources leave no doubt that the problems discussed for Russian society today are no less than relevant than for Western European countries and the United States. Russia follows the path of developed countries, albeit with some lag.
The reasons for the spread of excess weight in Russia are generally the same as in the whole world. Some difference - the “novelty effect” that accompanied in the early 1990s. the emergence of new consumer products on the market, a lack of information on the harmful properties of products such as fast food, carbonated drinks, etc. The lack of understanding by the majority of the population of the value of health and the priority of a healthy, active lifestyle, is also evident in relation to nutrition and sport. A recent survey by the Rosstat, “The Impact of Behavioral Factors on the Health Status of the Population”, showed that the share of those who in real life really save their health does not exceed 25% of those surveyed. In particular, 64.1% indicated that they do not comply with the diet; 76.4% do not do morning gymnastics; in fact, 18.8% of respondents are engaged in physical culture and sports. As a result, in recent decades we can observe in Russian society the same dynamics of growth of the average body mass index, as in other countries.
The consequences of overweight for human health in Russia also do not differ from those known in other countries: they are serious chronic diseases. So, a recent study by Ya.M. Roshchina on the data for 2000-2005. confirmed that the likelihood of hypertension, heart attack, other cardiovascular diseases and diabetes depends positively on the body mass index.
Before presenting our own estimates of prevalence and overweight factors, we define what we mean by abnormality. Researchers of this issue in most cases rely on the concept of body mass index - BMI. A deviation from the norm is considered to be a BMI> 25, and if a BMI is> 25, they are said to be overweight, if a BMI> 30 - about obesity. Thus, the concept of overweight is wider, and obesity is already. Specialists also identify certain groups of obesity (BMI> 35,> 40), or the so-called morbid forms. In our study, we will follow a slightly different methodology: we divide the entire population into three large subgroups - people of normal weight; overweight, but not yet in the stage of obesity (30> BMI> 25), and suffering from obesity (BMI> 30). Thus, our subgroups do not overlap, which simplifies further calculations and comparisons.
The empirical analysis presented in this section is based on the results of the 15th wave of the Russian Monitoring of the Economic Situation and Public Health (RMEZ), which are dated 2006. Initially, 14,690 individuals were included in the sample. However, for the purposes of this study, only those respondents who answered the question about their weight and height are of interest. They turned out to be 91.6% of the total number of people surveyed (1236 people were excluded from the sample). In addition, in a number of studies, the problem of overweight and obesity is given special attention and a slightly different methodology is used for analysis. For this reason, only adult individuals over the age of 18 are in our sphere of attention. As a result, the sample size was reduced to 76.7% of the original size, and ultimately amounted to 11265 people, of which 4803 are men (43%) and 6462 are women (57%).
On the basis of the data obtained, the average BMI was calculated for the entire adult population as a whole and separately for men and women.
From the data obtained it follows that in Russia the problem of overweight and obesity does exist, given that the average BMI value exceeded the threshold value of 25 and was 25.77. Moreover, it is obvious that for women the problem is more acute - the average BMI for them is 26.28 (versus 25.08 for men). The median value of BMI shows that more than half of women in our country are experiencing difficulties associated with overweight. It is also interesting that the spread of BMI values relative to the average for women is higher than for men, as evidenced by the value of the standard deviation - 5.81 versus 4.17, respectively. This fact allows us to conclude that women with a significant imbalance of height and body weight can be found more often than men with the same problem.
In order to understand the scale of the problem of overweight in Russian society, we estimated the absolute and relative number of people suffering from overweight and obesity.
According to the WHO, the problem of overweight in Russia really causes concern. Our calculations based on RLMS data give comparable estimates37. Namely, about a third of both men and women are overweight.
Obesity is a less common problem: more than 12% of men and about 25% of women suffer from it. Thus, in general, we obtained that 49% of the entire Russian population suffers from overweight (44.5% of men and 52.3% of women).
The presented estimates indicate the scale of the problem of overweight in 2006. At the same time, our research suggests that a steady tendency to weight gain has developed in Russia, so that over time, the problem under consideration will most likely be exacerbated. From 1996 to 2006, we calculated the average BMI values and the proportion of adult respondents who are overweight and obese on the RLMS waves.
It can be seen that for almost the entire period from 1996 to 2006. there was a positive increase in both the average BMI and the proportion of overweight and obese people.
To understand which age groups are more affected by overweight or obesity, we have divided the sample into 6 age groups. Judging by the results, the problem of overweight in society in principle arises after reaching the age of 30 years: by this time the average value already exceeds the permissible threshold of 25, but the median does not exceed the critical value. Every second person begins to suffer from overweight after 45 years, when the median value exceeds 25.
As can be seen, after 30 years, the average BMI for women is always higher than the average BMI for men. The most at risk associated with overweight, women aged 60 to 69 years, as clearly indicated by both the average and median values of BMI, the values of which are close to the mark signaling obesity. The same age can be called critical for the male part of the population. After 70 years, the problem of overweight is not so acute.
The non-monotonous nature of the resulting dependence of BMI on age can be explained, in our opinion, by two main reasons:
- Firstly, overweight in Russia, as in other countries of the world, is a relatively new and growing phenomenon, and therefore more typical for the middle-aged population than for the elderly. Food addictions and lifestyle of the elderly were laid much earlier and have not undergone such a strong change in recent years as in the younger generations;
- secondly, serious diseases and relatively early mortality of people suffering from obesity, lead to the fact that in the older age cohorts they are physically less and less (the same is true for alcoholics and smokers). This means that the average BMI in these age groups decreases as more people disappear naturally.
We were also interested in whether there is any connection between the prevalence of overweight and the education of the respondents, because foreign studies emphasize the primary importance of this factor, namely, the steady negative dependence of BMI on the level of education received. It turned out that the Russian situation looks qualitatively different. We identified four main groups of respondents who received incomplete secondary education, completed secondary education, completed secondary vocational education, and higher or postgraduate professional education (the group of respondents with primary education is too small in our sample).
The situation for men and women is radically different. If among women with higher and postgraduate education, the proportion of obesity is indeed significantly lower (18% versus 24-29% in groups with incomplete and completed secondary education), then in men there is an obvious opposite trend. The higher the level of education, the more in the corresponding group of those whose BMI is higher than the norm (and this is true for overweight and for obesity). To test the significance of the results obtained, we estimated the correlation between BMI values and education levels by groups of respondents (for men, women, and for the entire sample) using the Pearson coefficients.
Although the values of the coefficients and small in absolute values, the relationship is statistically significant, and for men is positive, and for women - negative. Thus, the relationship of weight and education in Russian society cannot yet be unambiguously assessed.
Estimates of the economic costs of overweight and obesity in Russia
We tried to show the existence of direct and indirect costs of excess weight in the Russian economy. In this regard, we have put forward two hypotheses:
- Individuals with excess weight, receive a relatively lower labor income. The indirect costs of being overweight can be either in the form of relatively low wages (productivity) or in the form of wage losses due to absence from work due to illness.
- The direct costs of overweight come in the form of higher costs for the treatment of diseases (in particular, in the form of more frequent visits to doctors).
Hypothesis Test #1
First of all, we wanted to understand whether there is a negative relationship between the salary of an employee and his body weight, that is, whether it is possible to estimate in this way the indirect costs due to the lower productivity of the employee. For the analysis, as before, the data of the 15th wave of the RLMS for 2006 were used. We took only the data of those respondents who worked for the calculations: the subsample was 5689 people. As a dependent variable, two options for estimating the salaries of respondents were selected:
average monthly salary of an individual (W);
- the hourly wage of the individual (Aver_W).
In the role of independent variables were used:
- BMI - body mass index,
- BMI ^ 2 - squared body mass index;
- AGE - age of the individual,
AGE ^ 2 - the square of the age of the individual. The following regressions were evaluated38
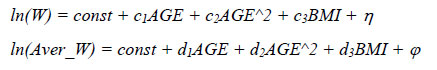
The results did not confirm our hypothesis. Estimates of the models make us, with a high degree of probability, assert that at the time of the survey there was a positive relationship between the size of an individual’s salary and his body weight. The existence of a positive relationship between wages and a person’s weight is also confirmed by a matrix made up of partial correlation coefficients. We also tried to look at the possible link between earnings and weight in terms of gender groups, believing that for men and for women dependencies may turn out to be different. Indeed, the positive relationship was statistically significant only for men, while for women, the corresponding regression coefficients for the BMI variable turned out to be insignificant.
As the results of calculations show, the salary in Russia significantly depends on the age of the employee, and at first positively, and then negatively. Previously, we found a parabolic relationship between body mass index and the age of an individual. This suggests that the BMI has a quadratic relation with wages. To test this hypothesis, we constructed models of the following form:
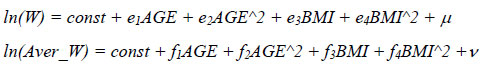
Indeed, the estimates obtained confirmed our assumption that there is a quadratic relationship between salary and BMI. This suggests that in reality, perhaps, there is a certain threshold level of weight of the individual, after which the salary begins to fall. Then, the results of the evaluation of models (1) - (2) that we obtained indicate only that in 2006 the critical level of BMI was not achieved in society, and therefore the labor market reacted poorly to the excess weight of workers. However, given the trend of increasing the average BMI over the last decade, it can be assumed that in the future the labor market may begin to react negatively to overweight workers (“punish” workers). Note that this assumption is consistent with the opinion of foreign researchers, who have repeatedly noted the non-monotonous and bilateral nature of the relationship between wages and employee weight. Apparently, in Russian society, in contrast to developed countries, that threshold of income growth has not yet been passed, after which the BMI begins to decline as a result of targeted actions of individuals themselves.
Although the growth of BMI in Russia does not yet have a restraining effect on wages, it was possible to identify certain economic losses for society, however. RLMS data allow estimating indirect economic costs through underproduction due to temporary disability. So, working respondents were asked the question: "How many days have you missed due to illness in the last 30 days"? Absolute estimates (in days) may not be applicable to extrapolation to society as a whole, since only about 6% of working citizens (actually missing work due to illness during this month) answered this question.
At the same time, first of all, incremental indicators are important for us - the difference in the average duration of disability for people with overweight or obesity compared with people of normal weight. These incremental figures can be estimated in monetary terms if the average wage of an employee is used (assuming that wages are a reflection of productivity). According to Rosstat data for 2006, it amounted to 10,633.9 rubles per month, or 483.4 rubles per 1 working day. The data obtained are sufficient to calculate indirect losses from overweight.
To extrapolate the “incremental” loss in wages (productivity) of workers to the entire economy, we use Rosstat data on the average number of people employed in 2006 (67174 thousand people) and data on the BMI distribution based on RMEZ: 53.83% of people with a BMI <25; 28.82% of people with 30> BMI> 25; 17.36% of people with a BMI> 3040. Calculate the absolute number of three groups of workers with different levels of BMI. Then, multiplying the incremental wage losses by the number of overweight and obese workers, we obtain the total cash loss per month due to their longer incapacity for the entire economy. These losses can also be overestimated on the basis of a full year (more than 330 billion rubles) and, for clarity, compare with such macro-indicators as, for example, GDP or total government spending on health care in 2006. It turns out that only additional losses from longer working disabilities overweight and obesity make up 1.02% of the country's GDP, or 35% of the consolidated budget expenditures on health care (including MHI).
Test hypothesis #2
We tested the hypothesis of a positive relationship between a person's BMI and his treatment costs to confirm the direct costs of being overweight. As before, we relied on the RLMS database for 2006. The dependent variable was the frequency of visits to the doctor (N_Doc). In addition to the BMI, the former variables - AGE, AGE ^ 2 were used as independent, so we controlled age as one of the most important factors of morbidity. We estimated the regression of the form:
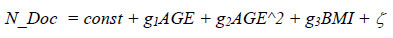
The results obtained confirmed our assumption that overweight is a significant risk factor for diseases, and therefore entails the need for more frequent access to medical care. The negative coefficient at the BMI variable shows that an increase in the weight of an individual reduces the rank of the variable N_Doc, and thus increases the frequency of visits to the doctor. The distribution of the average number of doctor visits per year also speaks against the benefit of obese people - the higher the BMI, the more often a person visits the doctor.
In other words, it can be argued that the negative sign of the coefficient at the BMI variable clearly reflects the direct economic costs of excess weight, since each additional doctor’s appointment is associated with expenses for the state, the insurance company or directly for the patient. Since the RLMS does not provide specific data on the number of visits to the doctor, but only suggests ranking values, we cannot accurately estimate the amount of additional direct medical costs for people with excess body weight.
Findings
The problem of overweight and obesity has directly touched Russian society today. Both absolute and relative indicators of BMI, and most importantly - their dynamics, indicate the need for close attention of policy makers to this problem. Among the direct and indirect effects are reduced productivity of workers, loss of working time, difficulties in finding employment, psychological costs, and most importantly, an increase in the incidence and associated costs - both for the individual and for society as a whole. In most developed countries, politicians and economists have long recognized the existence of this problem, state programs are being developed, detailed estimates of the burden of diseases caused by overweight and other types of economic costs are being carried out to substantiate specific health policy measures. In Russia, the authorities, as is often the case, prefer to deal with the consequences rather than the problem: they finance special programs and projects for the treatment of certain diseases, the cause of which in most cases is overweight. The very problem of overweight and obesity, unhealthy diet and lifestyle of the vast majority of Russians is not considered as a priority.
For the Russian economy, the data of the RLMS for 2006 do not allow us to reveal the negative impact of the excess body weight of an employee on his wages. We see the reason for this in the presence of a non-monotonous relationship between labor income and BMI and the as yet insufficient reaction of the labor market to deviations from the normal weight of workers. However, given the trend towards a permanent increase in BMI, in the foreseeable future we can expect some drop in wages of people suffering from overweight (as is the case in more developed economies).
However, we were able to show what kind of indirect economic costs a society already has at the moment - we estimated the scale of losses due to the temporary disability of people with overweight and obesity. We have shown that these losses are comparable to the general health budget (about one third). Thus, special programs to reduce body weight, will be economically justified if we compare the costs of them and the expected benefits (productivity gains). An unequivocal positive relationship was also established between BMI and the frequency of visits to the doctor, which indicates that there is an additional public burden associated with direct medical costs for treating people with abnormal body mass.
Summarizing what has been said, it can be concluded that according to our estimates, overweight and obesity in the Russian economy do have high economic costs. More detailed primary data (in particular, data from special surveys) would allow a more accurate estimate of total expenses in monetary terms, in particular, the additional costs of medicines, outpatient and inpatient care, caused by obesity. Today, such calculations are impossible precisely because of the lack of primary information, but for a serious justification of public policy measures such assessments are necessary.
 myfast
myfast AU
AU UK
UK CA
CA DE
DE FR
FR IT
IT ES
ES


